2011 is just wrapping up. It has been a great year, with many highs and only a few lows. I started my first blog this year and have been having a great time.
The question, "What was the best part of 2011?" has been flying around and I'd have to say, having my amazing family to spend every day with! This leads me to my "New Year's Resolutions," which happens to be summed up on an awesome picture I found at a favourite store yesterday...
January 1st, 2012 is the day the twins turn 20 months old, so Happy 20 Months to my boys! To my family, friends and readers, I hope you have a healthy and happy 2012! Happy New Year!
31 Dec 2011
15 Dec 2011
Christmas Spirit
I am getting this blog post in just under a month since my last posting. It has been a chaotic month with lots of changes, mostly for the better, but a stressful time.
Now that most of the stress is behind us I can focus on my favourite time of the year. Christmas! When it comes to Christmas I really do have a lot to be thankful for and I often think of the families that have children in hospital during this time. I am very glad we didn't have to experience our hospital stays during the Christmas season, as I feel that would have been an even harder period to get through. The NICU experience is hard enough, but to throw holidays or special times into the mix would be hard.
One thing I do know from speaking to families that delivered babies during the holidays and those that have spent it in the hospital or NICU, is that the hospitals do try to make the experience as positive and special as possible for the families there.
Hospitals always have amazing volunteers and donors sending in monetary gifts, quilts, blankets, baby caps, booties, toys and other special items for the children in the hospitals over the season. If you have a Christmas baby you are more than likely to receive a little bit of extra special attention because it is often a quieter time on the hospital wards.
I have seen and heard of great things sent into NICUs. Special care packages for the mom or dad or babies in the hospital. Cute onesies or hats made by donors. One very cute onesie I've seen says, "Ho Ho Home please," which I think is too cute. I've seen some adorable knitted Santa hats made for little preemie or termie babies. I am confident that a mother seeing one of these cute little items on their baby would feel extremely happy and well-supported by the kindhearted strangers that felt her family needed to feel like it is a special time regardless of the fact they are in the NICU. I only wish I had an amazing talent like knitting or crocheting, so that I could do something like this. Maybe one day...when life is less chaotic (will that ever be?)
Today we returned to our twins' first homebase and visited some NICU staff and dropped off a gift for two babies. We were told they'd probably go to a family with new twins, as there are a couple sets in the unit now, but they may go to two single babies, which is fine with us. These are the times I wish I had a million bucks (or two) so that I could outfit every deserving, cute little preemie and termie in the NICU and hopefully give their families that boost of support that I know they need. I think I am concocting a plan in my head already for next year...
Following our NICU visit we got to catch up with some of our "Home away from home" friends, who visited us in their comfy Family Room in the hospital. It is amazing how such a trying time can bring out new friendships and tight bonds that hopefully will last a lifetime. During this visit I was talking about our children's amount...or mountain...of toys that continues to grow and grow and how I've asked that friends and family not give the gift of toys for our children's Christmas. Some people have looked at me like I'm looney or Mrs. Scrooge, but the point I make is that our kids have lots of toys to play with and the money could be better spent elsewhere...whether it's a donation to a NICU, Labour & Delivery ward, an infant development program, centre for child development, family and children's services, etcetera., etcetera. There are lots of great places money or gifts can be directed to. When we were living at the Ronald McDonald House our family was showered with kind gifts and surprises for our sons and it only seems right that I focus attention on this constant need to ensure that families of today and tomorrow continue to get the support and brighter days because of unexpected, fun surprises during what can be a dark and scary time.
Now is a great time of year to pick a new cause and provide a donation to it. If you can't afford a monetary donation, you can donate your time, your skills, your hobbies and put your own personal stamp on the way you choose to help out. The best part is that whatever method you choose there will always be a smiling and thankful person at the other end. This is what I believe is the meaning of, "Christmas spirit."
Now that most of the stress is behind us I can focus on my favourite time of the year. Christmas! When it comes to Christmas I really do have a lot to be thankful for and I often think of the families that have children in hospital during this time. I am very glad we didn't have to experience our hospital stays during the Christmas season, as I feel that would have been an even harder period to get through. The NICU experience is hard enough, but to throw holidays or special times into the mix would be hard.
One thing I do know from speaking to families that delivered babies during the holidays and those that have spent it in the hospital or NICU, is that the hospitals do try to make the experience as positive and special as possible for the families there.
Hospitals always have amazing volunteers and donors sending in monetary gifts, quilts, blankets, baby caps, booties, toys and other special items for the children in the hospitals over the season. If you have a Christmas baby you are more than likely to receive a little bit of extra special attention because it is often a quieter time on the hospital wards.
I have seen and heard of great things sent into NICUs. Special care packages for the mom or dad or babies in the hospital. Cute onesies or hats made by donors. One very cute onesie I've seen says, "Ho Ho Home please," which I think is too cute. I've seen some adorable knitted Santa hats made for little preemie or termie babies. I am confident that a mother seeing one of these cute little items on their baby would feel extremely happy and well-supported by the kindhearted strangers that felt her family needed to feel like it is a special time regardless of the fact they are in the NICU. I only wish I had an amazing talent like knitting or crocheting, so that I could do something like this. Maybe one day...when life is less chaotic (will that ever be?)
Today we returned to our twins' first homebase and visited some NICU staff and dropped off a gift for two babies. We were told they'd probably go to a family with new twins, as there are a couple sets in the unit now, but they may go to two single babies, which is fine with us. These are the times I wish I had a million bucks (or two) so that I could outfit every deserving, cute little preemie and termie in the NICU and hopefully give their families that boost of support that I know they need. I think I am concocting a plan in my head already for next year...
Following our NICU visit we got to catch up with some of our "Home away from home" friends, who visited us in their comfy Family Room in the hospital. It is amazing how such a trying time can bring out new friendships and tight bonds that hopefully will last a lifetime. During this visit I was talking about our children's amount...or mountain...of toys that continues to grow and grow and how I've asked that friends and family not give the gift of toys for our children's Christmas. Some people have looked at me like I'm looney or Mrs. Scrooge, but the point I make is that our kids have lots of toys to play with and the money could be better spent elsewhere...whether it's a donation to a NICU, Labour & Delivery ward, an infant development program, centre for child development, family and children's services, etcetera., etcetera. There are lots of great places money or gifts can be directed to. When we were living at the Ronald McDonald House our family was showered with kind gifts and surprises for our sons and it only seems right that I focus attention on this constant need to ensure that families of today and tomorrow continue to get the support and brighter days because of unexpected, fun surprises during what can be a dark and scary time.
Now is a great time of year to pick a new cause and provide a donation to it. If you can't afford a monetary donation, you can donate your time, your skills, your hobbies and put your own personal stamp on the way you choose to help out. The best part is that whatever method you choose there will always be a smiling and thankful person at the other end. This is what I believe is the meaning of, "Christmas spirit."
17 Nov 2011
Different Shades of Purple
Today is November 17. It is one of the coldest days in my area of Canada so far and the snow began to fall lightly this morning.
In I went to work, armed with some purple icing covered cupcakes and all decked out in my favourite purple sweater. In came my colleagues. Hiding under their winter coats, which have recently been pulled out of the darkness of their closets, were different shades of purple.
We had colours of plum and eggplant, magenta purpley-pink, mauve and even some Barney The Purple Dinosaur purple...and some pink, because that's close to purple, right?? :)
By 9:00 there were several of my colleagues, also my friends, proud to wear purple to support the First World Prematurity Awareness Day.
By about 9:01, there we all were hovering around the kitchen table chowing down on purple coloured cupcakes with baby blue and pink diaper pins adorning them.
Through the tough times my family, friends and co-workers stood by me. My new co-workers who arrived on scene after I made my quick exit from my work duties when my twins arrived 13 weeks early, have come to know my story and support me equally. It is amazing to have such a support network and I can't say thank you enough.
Then we jumped off that rollercoaster and got right onto a new ride, taking us in the direction of home, which still has many ups and downs, bumps and jolts, but it is where we want to be and it couldn't be more exhilerating!
Not a day goes by that I don't feel thankful for the wonderful work of the neonatologists, the nurses and NICU staff that got us through that ride safe and sound.
We, as preemie parents, also have to thank organizations like the Linden Fund, here in Ontario, Canada, and the wonderful March of Dimes, that have gone to great lengths to get funding, supports and assistance for premature children and their families. This can be one of the toughest times a family can face and these types of organizations found all across the world make the "ride" feel a little saner.
Thank you for recognizing and raising prematurity awareness today and every day!
13 Nov 2011
Diaper Backward Spells Repaid...
Diaper backward spells "repaid." Seriously. I'm being repaid twofold! I must have really put my parents through a lot of crap during my diaper days!
I have been told many a time that as a toddler I used to take off my diapers aftering waking from my naps and would proceed to wipe the poopy ones on bedroom walls at home and the babysitter's. Oh my! Gross. I proceeded to teach my younger brother how to carry on the tradition when he was capable.
Talk about karma! Once the babies were home we were going through about 16-20 diapers a day. It got to the point I was dreaming of diaper change times because that's all it seemed I was doing in the early days.
When it comes down to it, diapers have been a big part of our lives. I'm not sure that everyone gets excited about the first time a diaper is put on their baby. I do know that as new parents many are afraid or not sure how to change their baby's first few diapers, but most dive in and figure it out.
When it comes to the NICU experience, a diaper is not always the first thing put on a baby. Instead it's leads and monitors and sticky tapes, breathing apparatuses and who knows what else? Then the diaper might come. There may not be a diaper that actually fits this "newborn" baby.
 |
| The Stages of Diapers of the Twins: Preemie Small, NB, 1, 2 & currently in 3. You can see the # "7" written on the Preemie diaper on the left, which I explain in this post. |
In all 3 of my cases, my babies were born suddenly and in an ill-prepared hospital without a NICU on site, therefore there were no teeny tiny diapers to put on their tiny new bodies. In each case, however, the size of the diaper was the least of anyone's worries.
Preemie #1 was transported to an appropriate unit and one of my first memories of him was him spread out on a warming bed in a very big diaper, pretty much swallowing up his lower body and torso. It was on very loose to avoid irritating his premature skin.
If I thought Preemie #1 was swimming in his first diaper, I was rudely corrected when Preemie #2 and Preemie #3 arrived. These two were more than 2 pounds less than their big bro. Finding ourselves in the "wrong" hospital again, they were not equipped with anything less than the standard newborn diapers.
Once the twins arrived at their NICU, on went the tiniest diapers I have ever seen! Pampers Premature Small. Wow. It amazed me that diapers were made this small! These diapers weigh 7 grams.
How do I know how much a diaper weighs and why do I know this?? Well, in the NICU a baby's bodily functions are monitored every 3 hours or less. The nurses in the unit will hand write "7" or whatever the weight of each diaper on the front to indicate how much the diaper weighed before the baby did his business in it.
 |
| My Cabbage Patch Kid "Preemie," Circa 1985. His leg is the same size as my 2 lbs Preemies' diaper! The "Preemie" is in a NB size diaper rolled up. |
Why would we want to weigh the diaper after the baby has worn it? To be pretty certain that the baby's fluid intake and urine output are balanced. Bloodwork and other assessments are carried out too in order to monitor the baby's nutrition, but one of the first obvious indicators of problems appears or does not appear in the diaper.
When it comes to changing a premature or NICU baby's diaper it can be outright terrifying for the parent. As premature babies' parents we are facing wire leads, tubing, monitors, machines, sticky things, tape, and a fragile baby connected to it all. We must stand outside the incubator, putting what are most likely gloved hands and arms through two small access holes to be able to work with the baby. It sucks learning to change a diaper for the first few times for any person or parent, but throw in an incubator and the awkwardness of manoeuvering through all of the wires and the fear of harming the baby and it can be a pretty terrifying, albeit very memorable experience.
Tonight I'm reminiscing about diaper changing for a particularly good reason. This month is Prematurity Awareness Month in the United States and November 17, 2011 is the First World Prematurity Awareness Day. A fellow preemie parent is currently working on "40 Diapers. 40 Days," to help create premature birth awareness and raise funds for a NICU in Haiti. She is painting 40 diapers and taking donations and a silent auction will be held at the end of 40 days.
I know what a scary and trying time the NICU process is, but can only imagine how much more difficult it would be living in a situation where a NICU is not the norm and most likely unattainable for most babies born too soon.
If you can, please visit her site at http://www.thepainteddiaper.com/ and support her along the way.
This Thursday, November 17, please wear purple to show support and help raise Prematurity Awareness! It's not talked about enough.
Thank you.
9 Nov 2011
Liebster Blog Award
So after a few moments of thinking about it, I confirmed in my head that, yes, it definitely is Wednesday. I seriously had to think about this for a few minutes and confirmed it by seeing what was on the T.V. tonight. If Modern Family is on, I know it's Wednesday. Unfortunately, I didn't actually get to catch the show, as my oldest son was just settling down for the night at the beginning of the show.
So given the fact that it is Wednesday, I considered making this my very first "Wordless Wednesday" post...BUT I figure my opportunities to get on here to blog have been few and far between since getting back into my full time job (aside from my full time job as Mommy,) so I want to make full use of my time...nevermind that it happens to be Wednesday. My first Wordless Wednesday can wait!
Then I realized I could have a "Wine Down Wednesday," but there is no wine, so I settled for a hot chocolate and a wordy blog.
Way back on October 7, I received a comment from a fellow blogger, Sharon, at http://mammadoitall.blogspot.com/, who let me know she had awarded me with the Liebster Award for bloggers. She listed me with four other bloggers, as blogs she was enjoying reading and following. How nice is that? It really did put a smile on my face to know that a woman in Manhattan, a journalist, was enjoying my writing and passing it on. So I am going to pass it on now...but it is going to be a two parter (mainly due to lack of time tonight.)
So given the fact that it is Wednesday, I considered making this my very first "Wordless Wednesday" post...BUT I figure my opportunities to get on here to blog have been few and far between since getting back into my full time job (aside from my full time job as Mommy,) so I want to make full use of my time...nevermind that it happens to be Wednesday. My first Wordless Wednesday can wait!
Then I realized I could have a "Wine Down Wednesday," but there is no wine, so I settled for a hot chocolate and a wordy blog.
Way back on October 7, I received a comment from a fellow blogger, Sharon, at http://mammadoitall.blogspot.com/, who let me know she had awarded me with the Liebster Award for bloggers. She listed me with four other bloggers, as blogs she was enjoying reading and following. How nice is that? It really did put a smile on my face to know that a woman in Manhattan, a journalist, was enjoying my writing and passing it on. So I am going to pass it on now...but it is going to be a two parter (mainly due to lack of time tonight.)
The following blogs are ones I enjoy reading when I get a chance and I hope you'll check them out too.
Changing Diapers and Taking Names at http://findingbrittnemo.blogspot.com/
This blogger hosts Blog Hops, which I love, as do many other bloggers out there. Blog Hops for those that don't know are intended to help bloggers find other bloggers within their own niche or other interests/hobbies. She also has a Mom of the Month tab, on which readers can nominate extraordinary moms. Very cool.
Mom is the Only Girl at http://momistheonlygirl@blogspot.com
This is a fun mother, who makes life interesting for her two boys. It seems like she and her husband set out to teach their boys something new every day in fun and interesting ways.
A Mommy Blog Design Studio at http://www.amommysblogdesignstudio.com/
This is a business, however, I do like her blog posts on the topics of how to make blogs work, especially for all us mommy bloggers out here. Not only does she provide good information, but she also has fun designs and blog packages that can be purchased.
I'm going to name two more, but not now...it's 11:30 and I am exhausted!
26 Oct 2011
Social Media/Work/Life Balance
It used to be those that work had the goal of having "work/life balance." Meaning we all strive to have a job and also be able to have a life outside that job. Just when I think I get a handle on this concept and have a pretty good balance going on, in comes social media and all its distractions and interesting things to read, comment and blog on.
I have been pretty in tune with computers, Internet and the ins and outs, fads and changes of social media since the early days of Internet useage. I have had the pleasure of working for two very well known computer software and telecommunications companies, giving me even more opportunity to learn about the emerging technologies, all the while being paid to do it.
I remember getting excited when Windows 95 came out and getting a new computer with it installed. I remember getting dial up and my very first email address. I remember my first hotmail account, which still exists and is used often. I remember ICQ and all the chats that stemmed from it and the ability to start conversations, drop them and return to them days later like it was nothing. I had Yahoo Messenger, MSN Messenger, AIM (AOL,) and ICQ running pretty much simultaneously and it was becoming the norm to chat online rather than chat on the phone. These were all a sign of many things to come.
I started using Facebook in 2007 and I think I was a pretty late bloomer on that. I tried to put it off and "rebel" against the latest thing, but eventually I began using it to communicate with close friends and family about upcoming wedding plans, and then plans for baby, and so on. It quickly became the quickest and easiest way to connect with a number of people, rather than have to make numerous phone calls or emails and hope that the message would be recieved.
This year I have created a blog, setup google +, started perusing Pinterest, created a Facebook Page (but haven't done anything with it yet,) and signed up on Twitter. Can you say, "information overload?" Yet this is the new norm. It's a little bit crazy when you think of it and it can become overwhelming to some.
For me, information is power. I enjoy taking on these challenges and learning as much as possible and then moving on to the next interesting thing. The downfall is that there are so many new, cool things going on, it's hard to keep up! That's when it can become overwhelming.
This is where social media/work/life balance come in. I began my blog while off on mat leave and able to take a few minutes to write during quiet time during the day when babies were sleeping or after they'd gone to bed in the evening. I could post 2-3 blogs per week if I felt like it.
I have been back to work almost 2 months, and let me tell you, opportunities to blog have become very difficult to find during my hectic day.
Monday to Friday look like this:
Wake around 5:45 or 6.
Get all 3 kids out the door by 7:45 (Hubby and I might have eaten, but probably not!)
Drop off at two different daycares by 8--One car goes one way, the other car another way.
Get to work by 8:30.
Work till 5:00.
Pick up kids by 5:30.Get home, make dinner, eat dinner by 6:30 or 7:00.
Play with kids 7:00-8:00.
Get kids in bed 8:00-8:30.Maybe login to FB and check out what's up in my social world 8:30ish
Around 8:32 realize I can't sit down because there are at least 6 bottles/sippy cups to wash, dishes to be cleared from table and thrown in dishwasher, etc., etc.Around 9:15 the above might be done. My back may be killing me. This is when I may get myself back onto Facebook or set myself up here infront of my blog. Or maybe I will actually try to watch one tv show in full, without interruption...but probably not!
Right now I can see that there is a serious imbalance between social media, life and work.
I'm working on it! I've been able to attend two workshops in the past week on the topic of blogging and Facebook for business. The facilitators suggest at least 2 blogs per week to maintain a blog. I would have to agree. It seems like it might be hard to do this every week, but the bottom line is I am answering to myself and a blog for me is something to be enjoyed and not felt as though it's another "job." I met a lady this week who said she had a "mommy blog" for four years and finally decided to give it up because it was taking her away from other things, especially family, and she became overwhelmed.
I don't want to get to feeling like she did. I am now thinking forward about how I would like to see these three great parts of my life balance out and each part be something I can enjoy and bend and flex with, as times and needs change.
To be continued...
13 Oct 2011
Occupational Therapy and TOYS!
I have found myself infront of the computer again tonight because the eldest boy has taken over and has his cartoons on the TV before going to bed. This is my way of tuning out the same cartoon he's seen at least 10 times!
I've said before that I'd rather browse around online, read the news, the daily gossip, browse other blogs and whatever else I stumble across. This is my way to unwind. Tonight while checking out what's going on in the world, I learned it is National Occupational Therapist Month in Canada (and other countries.)
Prior to my introduction to the World of Preemies, I knew the basics of what an Occupational Therapist was, but I did not know they also worked with newborn babies. My concept of an OT was that they worked in some form of rehabilitation for individuals who have suffered illness or injury and required one-to-one help with re-learning physical life skills.
Thankfully we have access to many options and services for our boys. We have been able to work with a particular children's centre for development and so we have had the privilege of having two different OTs, who focus on different areas of our twins' development.
I've said before that I'd rather browse around online, read the news, the daily gossip, browse other blogs and whatever else I stumble across. This is my way to unwind. Tonight while checking out what's going on in the world, I learned it is National Occupational Therapist Month in Canada (and other countries.)
Prior to my introduction to the World of Preemies, I knew the basics of what an Occupational Therapist was, but I did not know they also worked with newborn babies. My concept of an OT was that they worked in some form of rehabilitation for individuals who have suffered illness or injury and required one-to-one help with re-learning physical life skills.
Our first introduction to an Occupational Therapist was during our first NICU hospital stay with Preemie #1. We met with her a few times to discuss how to avoid "Flat Head Syndrome." Yes, that's a real thing! The technical term is "Plagiocephaly." Say that 5 times fast! The OT discussed how to use blankets rolled up and positioned in a manner that would help prop him while he slept to avoid him favouring one side or the other. She showed us how Preemie #1's head shape was showing signs he'd been favouring one side and how we could work to pretty easily correct it. He now has an awesomely shaped head, if I do say so myself.
Our second/third experience was Round #2 in a different NICU with Preemie #2 and #3 (AKA: Twin A, Twin B.) This time around we had very different needs, with two very different little babies. I would say Occupational Therapy began in the very early days of our 27 weekers' lives. The simple things like positioning the baby, draping them on their tummy in their isolettes was one of the first things done. Positioning them from side to side, as we did with their older brother.
Then came our introduction to Hydrocephalus. This is where the greater scope of Occupational Therapy kicked in. Now our one boy had been diagnosed with Hydrocephalus and the OT stepped in to assist with propping with special pillows to attempt to assist with flow of the cerebral spinal fluid...I guess I should say, to help alleviate some of the swelling of the head.
 |
| Getting ready to come home. |
After our little man's first surgery, we were introduced to the "butterfly pillow," which looks like a butterfly. The baby's head/upper back are placed into the butterfly's centre and the wings basically envelope around the baby's head, giving him a soft, comfortable place to rest his head. Pillows aren't usually used in the NICU in the isolettes or cribs. Once the baby had his second surgery, his VP shunt inserted, he really needed the butterfly pillow. In the first few days the baby showed obvious signs that his head hurt if we touched it or when moving him around, therefore being able to prop him on his pillow and build up behind the pillow we could angle him on the opposite side, taking pressure off his sore little head where the new shunt was. It's amazing what a simple little idea can help with. These are the ideas of Occupational Therapists and the families they work with.
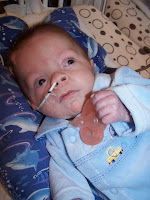 |
| Propped on a Butterfly Pillow NICU Discharge Day, August 20, 2010 |
We were fortunate to work with two different OTs while in our second NICU stay. The two of them sometimes would meet with me and we would collaborate and think of the best way to handle whatever situation had come up.
After surgery number two, the little man decided he didn't want to be bottle fed or breastfed and started to cough, choke, sputter, every time we attempted a regular feed, and he basically freaked me out! This is when you could say some "hard core" occupational therapy began. The OT scheduled during this period worked hard to help me work with the baby and think of how to overcome this latest obstacle to getting discharged from the hospital. No baby can be discharged if they are unable to eat and continue to gain weight.
We tried smaller amounts of expressed breast milk from a bottle, we tried formula, we tried a combination, we tried just nursing, we tried just bottling...We tried thickener put in with the EBM or formula. This boy had attitude and he didn't want to have anything to do with any of it! The OT was so helpful and rational. She would schedule to come in during one of his feeding times and feed him herself. She would try re-positioning him during the feeding time. Holding him in different ways to see how he responded. In the long run, it was a combination of her hard work, my work and everyone's overall determination and just a matter of time for him to figure it out again. For a period of time we chose to let him rest and he had a NG tube re-inserted to assist with feeds and help him continue to gain weight.
Eventually we all figured it out and he began to come around. He was discharged home with a NG tube and only a few days later it was out. Once home in the comfort of our own space, he caught on to eating well and never looked back.
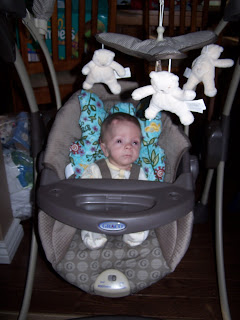 |
| Twin B Home and propped up with his new Butterfly Pillow, courtesy of The Linden Fund. |
Once discharged from the hospital we didn't lose our connection to the fascinating world of Occupational Therapy. We had the privilege of being connected with another OT through our local community and health care program. This OT paid us visits on a weekly basis to assess Twin B's progress and any other concerns that popped up. She assisted him with physical activities, eating habits and other ideas to help me help him. For example, we eventually graduated him to his high chair for meal times, along with his twin brother. He slumped over in his high chair and looked completely lost in the chair. Our OT came in and assisted with the best positioning and propping to get him comfortable for mealtime. It's amazing what a coffee towel and some bath towels can do!
The concepts that OTs use at times may seem simple, but to an over-tired mother and father, these simple things to try most likely won't click in our minds. When you think of it, the techniques OTs sometimes use, as simple as they are, aren't really things the average parent ever has to worry about and therefore it probably doesn't come naturally to most.
Eventually I noticed Twin A was definitely falling behind for hitting the many milestones, so he was able to work with the same OT in the home. She would exercise both babies, assist with their basic motor functions and see how well they were grasping cause and effect and basic reasoning abilities.
Thankfully we have access to many options and services for our boys. We have been able to work with a particular children's centre for development and so we have had the privilege of having two different OTs, who focus on different areas of our twins' development.
Recently we were able to part ways with our first OT who had been with us since NICU discharge. The boys had mastered the skills she was hoping they would and they were discharged yet again. "Discharged" is a nice word. Music to my ears.
We continue to work with our second (technically fourth) OT, who works on both boys' motor skills, assessing their abilities and working with them to figure out new ways to teach them and ensure they don't fall too far behind. This OT gets to play with toys and the boys. Who wouldn't want a job where you get paid to play with toys and babies?? Although it may seem like innocent and simple playtime to the average bystander, to a mother and an OT, it is a time for assessment, planning and implementation of concepts and ideas to assist the boys in becoming stronger, smarter and capable little boys.
 |
| One of our favourite toys at OT sesssions and at home! Simple, but fun! |
I've learned to look at toys and figure out what the true value of the toy is. Does it help my kids' fine or gross motor skills? Does it teach them cause and effect? Is it pretty much a useless toy, that I don't want to waste my money on? I've found that some of the simplest toys are the best toys for playtime. Toys don't need all the bells and whistles to be a good toy. I never would have thought about these things without the help of our Occupational Therapists.
So this month I am very thankful for our Occupational Therapists and I'm glad to recognize October as Occupational Therapists Month! They deserve it!
Thank you Carolyn, Auna, Veronica and Herdip. Awesome Occupational Therapists!
9 Oct 2011
We Are Lucky and Thankful!
This weekend is our Thanksgiving holiday. We celebrate with the usual turkey, ham, mashed potatoes and way too many sweets for dessert. We are very lucky to have a big family and have at least 2 dinners during the weekend, sometimes 3 or 4. These are the people that have provided my family of five with so much love and support that we couldn't ask for more! We are lucky to be surrounded by such wonderful people.
When people ask me what I am thankful for, of course my first response is my three boys. My happy family. I am thankful for a whole list of people and organizations that never crossed my mind only a few years ago. I am thankful for having the opportunity to learn about my children's needs and having a better understanding of what it means to be a mother. If you had asked me this a few years ago I wouldn't have had such an in depth response or given it all that much thought.
I am also thankful for all of the connections of preemie parents, specialists, nurses and those that are interested in the goings on of a preemie family. I wouldn't have found most of these connections if it weren't for the Internet!
Yesterday, while checking out Facebook, I read a wonderful perspective of another preemie mother on her idea of why "we" are chosen to be the mothers or parents of premature children. She highlights the fact that as parents we take nothing for granted with our premature babies. We feel lucky and blessed to have these children to call our own.
Here is Elli Drukman's story:
Did you ever wonder how the mothers of premature babies are chosen?
Somehow, I visualize God hovering Earth, selecting his instruments for propagation with great care and deliberation. As he observes, he instructs his angels to take notes... in a giant ledger.
"Armstrong, Beth, son. Patron Saint...give her Gerard. He's used to profanity."
Finally, he passes a name to an angel and smiles. "Give her a preemie."
The angel is curious. "Why this one God? She's so happy." "Exactly," smiles God. "Could I give a premature baby a mother who knows no laughter? That would be cruel."
"But does she have the patience?" asks the angel.
"I don't want her to have too much patience, or she'll drown in a sea of self-pity and despair. Once the shock and resentment wear off, she'll handle it. I watched her today. She has that sense of self and independence so rare and so necessary in a mother.
You see, the child I am going to give her has a world of its own. She has to make it live in her world, and that's not going to be easy."
God smiles. "This one is perfect. She has just the right amount of selfishness. "
The angel gasps, "Selfishness! Is that a virtue?"
God nods. "If she can't separate herself from the child occasionally, she will never survive. Yes, here is a woman whom I will bless with a child less than perfect. She doesn't know it yet, but she is to be envied."
"She will never take for granted a spoken word. She will never consider a step ordinary. When her child says "momma" for the first time, she will be witness to a miracle and know it."
"I will permit her to see clear the things that I see - ignorance, cruelty, prejudice - and allow her to rise above them."
She will never be alone. I will be at her side every minute of every day of her life because she is doing my work as surely as she is here by my side."
"But what about her Patron Saint?" asks the angel, his pen poised in the air. God smiles. "A mirror will suffice.
This is our second Thanksgiving home with our twin boys and I am no less thankful than I was one year ago. In fact, I may be even more thankful, having been able to see my babies grow another year and seeing them begin to interact with each other and their big brother. Every day I am thankful and I tell them so.
When people ask me what I am thankful for, of course my first response is my three boys. My happy family. I am thankful for a whole list of people and organizations that never crossed my mind only a few years ago. I am thankful for having the opportunity to learn about my children's needs and having a better understanding of what it means to be a mother. If you had asked me this a few years ago I wouldn't have had such an in depth response or given it all that much thought.
I am also thankful for all of the connections of preemie parents, specialists, nurses and those that are interested in the goings on of a preemie family. I wouldn't have found most of these connections if it weren't for the Internet!
Yesterday, while checking out Facebook, I read a wonderful perspective of another preemie mother on her idea of why "we" are chosen to be the mothers or parents of premature children. She highlights the fact that as parents we take nothing for granted with our premature babies. We feel lucky and blessed to have these children to call our own.
Here is Elli Drukman's story:
Did you ever wonder how the mothers of premature babies are chosen?
Somehow, I visualize God hovering Earth, selecting his instruments for propagation with great care and deliberation. As he observes, he instructs his angels to take notes... in a giant ledger.
"Armstrong, Beth, son. Patron Saint...give her Gerard. He's used to profanity."
Finally, he passes a name to an angel and smiles. "Give her a preemie."
The angel is curious. "Why this one God? She's so happy." "Exactly," smiles God. "Could I give a premature baby a mother who knows no laughter? That would be cruel."
"But does she have the patience?" asks the angel.
"I don't want her to have too much patience, or she'll drown in a sea of self-pity and despair. Once the shock and resentment wear off, she'll handle it. I watched her today. She has that sense of self and independence so rare and so necessary in a mother.
You see, the child I am going to give her has a world of its own. She has to make it live in her world, and that's not going to be easy."
God smiles. "This one is perfect. She has just the right amount of selfishness. "
The angel gasps, "Selfishness! Is that a virtue?"
God nods. "If she can't separate herself from the child occasionally, she will never survive. Yes, here is a woman whom I will bless with a child less than perfect. She doesn't know it yet, but she is to be envied."
"She will never take for granted a spoken word. She will never consider a step ordinary. When her child says "momma" for the first time, she will be witness to a miracle and know it."
"I will permit her to see clear the things that I see - ignorance, cruelty, prejudice - and allow her to rise above them."
She will never be alone. I will be at her side every minute of every day of her life because she is doing my work as surely as she is here by my side."
"But what about her Patron Saint?" asks the angel, his pen poised in the air. God smiles. "A mirror will suffice.
I think this is a beautiful story and a great answer to the "Why did I have a premature baby? Why me?" which I am sure most premature babies' mothers ask themselves.
This is our second Thanksgiving home with our twin boys and I am no less thankful than I was one year ago. In fact, I may be even more thankful, having been able to see my babies grow another year and seeing them begin to interact with each other and their big brother. Every day I am thankful and I tell them so.
22 Sept 2011
Hydrocephalus and The Future
When we found out about our son having hydrocephalus we tried to focus on the information provided by our doctor. We didn't alert the masses to tell them what had transpired a couple of days after his birth. Firstly, we didn't want the stress of trying to explain what was going on, over and over to friends and family. Secondly, we didn't want people researching the condition and scaring us with their findings. Thirdly, we didn't want pity. And finally, we (I) didn't want negative energy being aimed at our little boy, negative thoughts, negative concerns, the scary what ifs, and so on. I wanted to try to remain as positive as possible, because I do believe that even 27 weeker little premature infants can feel and understand negativity.
Our direct family and a few friends were told about what had happened and our request to keep it private was upheld. It was good to have the support of our direct family, as that was what mattered most at that time.
Eventually, we did get on the Internet and started a bit of research at recommended websites and so did our family. The information really did freak out some family members. Given the fact the NICU only allowed us, the parents, in to be with the babies, it was very hard for the grandparents and uncles and friends to understand what we and Baby B were going through. How Baby B was looking, acting, family couldn't see this. Pictures reflected a very small baby, with a very enlarged head. These pictures were probably frightening to those who had not been able to see the baby with their own eyes and see he seemed to be fairing well.
In the long run, what we learned through information from the neurosurgeons, neonatologists and staff, was that each baby is different and hydrocephalus impacts each person differently as well. Some babies may never be able to speak or walk. Some babies will have long term, regular complications, whereas some babies have a corrective surgery and never have to go through it again.
After a surgery is done to complete a shunt insertion, for example, there is the risk of infection or malfunction.
For all of these things, only time will tell.
The neonatologist and neurosurgeons gave us stories of people with hydrocephalus growing up and living perfectly normal and happy lives. Telling us many will attend university and so forth.
They also told us that on a rare occasion hydrocephalics' bodies can actually heal themselves over time, blockages are cleared and the CSF begins to flow normally from the brain and up and down the spinal column. This seemed to be one of those stories being told to us just to try to make us feel better about the situation, yet it did give us hope.
Then one day this month, I met a lady who told me her son had hydrocephalus. "He does??" I exclaimed, "So does mine." She looked at me like I was speaking another language, taking in what I just said. I told her the basics of our experience and she was amazed, as I was basically describing her experience which had taken place 33 years ago. Her son was born at 28 weeks or so and he was found to have hydrocephalus very quickly while in hospital as well. He had a shunt inserted and had a few corrective surgeries by the time he was 3. She then told me he was monitored by a pediatric neurosurgeon while he grew up. At the age of 18 he was transferred to an adult neurosurgeon in Toronto. When she and her son met this new doctor he completed his assessment and ran some scans and revealed to them that his shunt was not working. Of course this worried them to hear this news, when all along they thought everything was fine. He then said something like, "Did Doctor So-and-so not tell you your shunt is not working and it doesn't need to work anymore because your body is working for you again?" I can only imagine the relief this mother would have felt! That is an amazing and inspiring story. I guess miracles do happen, dreams do come true and stranger things have happened.
I was able to meet this woman's son, who is the same age as me. I met him yesterday and was able to talk with him about how he felt when growing up. He told me he was not allowed to participate in contact sports, such as hockey. Growing up in Canada and not playing hockey might be challenging for a kid. He was not allowed to participate in any physical education activties and had to sit on the sidelines. He was told as a child he couldn't do these things for fear of shunt malfunction and/or getting hit in the head with a ball, bat, hockey stick, puck, whatever...He went on to tell me that he was often delayed in many areas his peers were not. They were hitting milestones at the right time and he wasn't. He said eventually it got to the point he felt very excluded from his classmates, he wound up sitting in the back of class because it was harder for him to learn some things and he began to dwell on his condition and found that to be very hard.
He gave me advice and that was to avoid treating our son as someone "different." To try not to over-protect and shelter him. To get him out and active in his community and let him try things (within reason.) He said he didn't blame his mother for over-protecting him, as she was young at the time, single and did her best to protect him and keep him well. He also pointed out times have really changed in 30 years.
When this man was born, his young, single, alone mother was told that it may be best to institutionalize him, as he would never walk, never talk and never be able to function like a "normal" child. She did not take the doctors' advice and said she was determined to prove them wrong. She did a very good job in proving them wrong, I think. He walks, he talks and is healthy overall. Then he goes and does the amazing and grows out of the need of his shunt.
He did tell me he finds it difficult sometimes dealing with math and that he does suffer from bi-polar disorder, which may or may not be attributable to some long term damage to his brain. No one really knows. He also had a mild shake in his hands.
He says he is happy to share his story, as he did live a hard life in many ways, and if he can help others along the way, then it's worth it.
I am very grateful to have met this man and I now have a very well-rounded knowledge of what can happen and how to overcome any obstacles that may come our way.
Our direct family and a few friends were told about what had happened and our request to keep it private was upheld. It was good to have the support of our direct family, as that was what mattered most at that time.
Eventually, we did get on the Internet and started a bit of research at recommended websites and so did our family. The information really did freak out some family members. Given the fact the NICU only allowed us, the parents, in to be with the babies, it was very hard for the grandparents and uncles and friends to understand what we and Baby B were going through. How Baby B was looking, acting, family couldn't see this. Pictures reflected a very small baby, with a very enlarged head. These pictures were probably frightening to those who had not been able to see the baby with their own eyes and see he seemed to be fairing well.
In the long run, what we learned through information from the neurosurgeons, neonatologists and staff, was that each baby is different and hydrocephalus impacts each person differently as well. Some babies may never be able to speak or walk. Some babies will have long term, regular complications, whereas some babies have a corrective surgery and never have to go through it again.
After a surgery is done to complete a shunt insertion, for example, there is the risk of infection or malfunction.
For all of these things, only time will tell.
The neonatologist and neurosurgeons gave us stories of people with hydrocephalus growing up and living perfectly normal and happy lives. Telling us many will attend university and so forth.
They also told us that on a rare occasion hydrocephalics' bodies can actually heal themselves over time, blockages are cleared and the CSF begins to flow normally from the brain and up and down the spinal column. This seemed to be one of those stories being told to us just to try to make us feel better about the situation, yet it did give us hope.
Then one day this month, I met a lady who told me her son had hydrocephalus. "He does??" I exclaimed, "So does mine." She looked at me like I was speaking another language, taking in what I just said. I told her the basics of our experience and she was amazed, as I was basically describing her experience which had taken place 33 years ago. Her son was born at 28 weeks or so and he was found to have hydrocephalus very quickly while in hospital as well. He had a shunt inserted and had a few corrective surgeries by the time he was 3. She then told me he was monitored by a pediatric neurosurgeon while he grew up. At the age of 18 he was transferred to an adult neurosurgeon in Toronto. When she and her son met this new doctor he completed his assessment and ran some scans and revealed to them that his shunt was not working. Of course this worried them to hear this news, when all along they thought everything was fine. He then said something like, "Did Doctor So-and-so not tell you your shunt is not working and it doesn't need to work anymore because your body is working for you again?" I can only imagine the relief this mother would have felt! That is an amazing and inspiring story. I guess miracles do happen, dreams do come true and stranger things have happened.
I was able to meet this woman's son, who is the same age as me. I met him yesterday and was able to talk with him about how he felt when growing up. He told me he was not allowed to participate in contact sports, such as hockey. Growing up in Canada and not playing hockey might be challenging for a kid. He was not allowed to participate in any physical education activties and had to sit on the sidelines. He was told as a child he couldn't do these things for fear of shunt malfunction and/or getting hit in the head with a ball, bat, hockey stick, puck, whatever...He went on to tell me that he was often delayed in many areas his peers were not. They were hitting milestones at the right time and he wasn't. He said eventually it got to the point he felt very excluded from his classmates, he wound up sitting in the back of class because it was harder for him to learn some things and he began to dwell on his condition and found that to be very hard.
He gave me advice and that was to avoid treating our son as someone "different." To try not to over-protect and shelter him. To get him out and active in his community and let him try things (within reason.) He said he didn't blame his mother for over-protecting him, as she was young at the time, single and did her best to protect him and keep him well. He also pointed out times have really changed in 30 years.
When this man was born, his young, single, alone mother was told that it may be best to institutionalize him, as he would never walk, never talk and never be able to function like a "normal" child. She did not take the doctors' advice and said she was determined to prove them wrong. She did a very good job in proving them wrong, I think. He walks, he talks and is healthy overall. Then he goes and does the amazing and grows out of the need of his shunt.
He did tell me he finds it difficult sometimes dealing with math and that he does suffer from bi-polar disorder, which may or may not be attributable to some long term damage to his brain. No one really knows. He also had a mild shake in his hands.
He says he is happy to share his story, as he did live a hard life in many ways, and if he can help others along the way, then it's worth it.
I am very grateful to have met this man and I now have a very well-rounded knowledge of what can happen and how to overcome any obstacles that may come our way.
21 Sept 2011
Hydro...what??
In the United States the month of September is Hydrocephalus Awareness Month. "Hydro...what?" you ask? Hydro-seff-ah-luss. I've recently read in other parts of the world it is pronounced, "Hydro-keff-ah-luss." However you pronounce it, it's still the same thing...a lifealtering, potentially deadly condition of the brain. Hydrocephalus comes from the Greek for "water on the brain."
This time, two years ago I wasn't yet into my second pregnancy. This time, two years ago I didn't know in 8 short months I'd be having twin babies born 3 months early. This time, two years ago I didn't know the word, "hydrocephalus."
Fast forward to May 3, 2010, our second full day in a Level III Neonatal Intensive Care Unit. I can recall this day, as though it happened only a few hours ago. I can recall my steps to the wash basin to clean up my hands. I can recall the hush in the unit as we entered our babies' bed area and the quick glance that came from our neonatologist, who was standing by Baby B's bed. I can recall my husband mumbling under his breath that this doesn't seem good. I remember trying to be optimistic, saying, "Maybe he just wants to update us on things?" More of a question than a statement.
The doctor briskly came toward us. He handled it well. He did not approach us in a rushed, worried manner. Instead he greeted us by first names and asked us to come into a private room. He was calm and collected. Of course, as soon as he invited us in to the private room, we knew we weren't being updated on the morning's routine details. He had a social worker in tow and the nurse on with the babies. Not a very good sign.
The doctor said that one of our babies had just experienced an intraventricular hemmorhage and pulmonary hemmorhage simultaneously. Hearing this was terrifying. The doctor advised us he had actually been at his bedside when the baby started to take a turn for the worse. The baby's appearance had quickly become very ashen (grey) and he appeared to become rigid. That's the way he described it. He didn't go into detail as to whether or not he had physically done something to try to help the baby through it, but realistically I'm not sure that anything can be done in such a situation, except to hope the baby pulls out of it.
As we were only two days into our long stay at the hospital, we were still taking the trip back home nightly, so we felt terrible knowing we were not there when one of our babies was going through one of the biggest challenges of his life at only 2 days old.
I think the shock of being told the details kept me and my husband calm. I rationally asked questions. Why does something like this happen? What does an ultrasound or xray show now? What's the prognosis?
We talked for probably a good forty-five minutes in the private room, just to the side of our twins' bedsides. The social worker took notes. The nurse ensured we understood the doctor's medical lingo and broke things down in layman's terms as needed. The doctor drew diagrams of the brain and the spinal column. He drew a normal brain and the ventricles and an example of how our son's was appearing. His was pretty much filled with blood from the hemmorhage. Now we had to wait and see if the body could naturally clear the ventricle. If the blood could not clear, surgery may be required. A VP (Veintriculoperitoneal) Shunt may need to be inserted by a surgical process.
I remember during this time, the sound of the monitor bell alarms going off was extremely distressing to me in my mind. I didn't want to be sitting in this closed off box of a room. I wanted to be at my twins' bedside and see how the one baby was looking. By this point he was less than the 2 lbs 4 oz he was when he was born. A tiny little skinny thing, with nothing but potential.
Right from the day we arrived in the NICU we had asked the doctor not to scare us with all the maybes, what ifs and possibilities of anything long term for our premature boys. Given this new chain of events, I really wasn't interested in knowing what the future may hold in connection with this new condition we were dealing with. I wanted to deal with the here and now and not the various possible outcomes. We repeated over and over again during our stay, "One day at a time," "One step at a time," "One step forward, two steps back." The third one is really depressing to think about, but various versions of that were said very, very often.
The next three months would be a rollercoaster ride of fear, tears, pride, smiles and at last, relief. Our little man had 2 surgeries before he was 2 months old...before he was even due. He was a fighter and continued to surprise everyone with his ability to recover.
Initially he had a ventricular reservoir inserted into his right front ventricle, which acted as a small place to hold excess cerebral spinal fluid (CSF) and help (a bit) to alleviate some of the intracranial pressure. The fact that the ventricle was blocked was causing the CSF to back up in the brain, causing head swelling. He somewhat resembled The Great Gazoo (you know, from the Flinstones?) His head circumference was enlarged because of the swelling and although it looked terrible, he seemed to be comfortable usually.
The intention of the reservoir was to help extract excess fluid by "tapping" the reservoir every now and then. The hope was that the reservoir would buy time for the body to heal itself. Every time the baby's head/reservoir was tapped, it ran the risk of exposing him to infection. Eventually it got to the point that doing reservoir punctures and lumbar punctures to extract fluid were not productive enough to make doctor's feel a VP Shunt was not needed. So just before his actual due date he had his second surgery and a VP Shunt was inserted.
After surgery he was awake as they wheeled him out in his tiny little plastic transport box on a stretcher. The doctors had said not to expect him to be awake for potentially several hours after the surgery, but there he was looking up at us as they wheeled him out. There was a huge sense of relief.
Unfortunately, about 3 days after his surgery he was so tired out from his surgery and having been put back on full feeds pretty much immediately after surgery (the same day.) It seems we pooped him out and he couldn't handle full feeds and all the energy he needed to keep them up. He was nursing with me and not on a bottle. Eventually, we had to take a nurse's recommendation and get him onto bottle feeds to help him pace himself and possibly be more comfortable at feeding times. He had begun to cough, choke, sputter and forget to breathe when he was nursing and/or bottling. It was so frustrating to have a baby who was nursing 100%, amazingly well the day before surgery, only to have a baby who now had to re-learn it all.
Eventually it got to be that he was losing weight and having such a hard time taking a bottle that he was burning more calories than taking in. At that point in went the NG (naso-gastric) tube into his nose and down to his tummy. Now he was back on "gavage" feeds, running his milk through a syringe and tube into his stomach every three hours. This was disheartning. Depressing. Frustrating. Yet, he began to gain weight again, so at least it was serving a purpose.
Slowly, but surely over another 3 and a half weeks, we worked at getting him to take a bottle and/or nurse effectively. It was a trying time, but I was confident in my skills as a mother and my son's strength, and knew that with the right amount of patience and the right environment we would be fine.
Wow, this is turning into a very long post. I have so much more to say...so I will have to do another blog very soon.
I will continue my story and discuss the discharge, as well as talk about meeting another individual with hydrocephalus who has beaten many odds...
This time, two years ago I wasn't yet into my second pregnancy. This time, two years ago I didn't know in 8 short months I'd be having twin babies born 3 months early. This time, two years ago I didn't know the word, "hydrocephalus."
Fast forward to May 3, 2010, our second full day in a Level III Neonatal Intensive Care Unit. I can recall this day, as though it happened only a few hours ago. I can recall my steps to the wash basin to clean up my hands. I can recall the hush in the unit as we entered our babies' bed area and the quick glance that came from our neonatologist, who was standing by Baby B's bed. I can recall my husband mumbling under his breath that this doesn't seem good. I remember trying to be optimistic, saying, "Maybe he just wants to update us on things?" More of a question than a statement.
The doctor briskly came toward us. He handled it well. He did not approach us in a rushed, worried manner. Instead he greeted us by first names and asked us to come into a private room. He was calm and collected. Of course, as soon as he invited us in to the private room, we knew we weren't being updated on the morning's routine details. He had a social worker in tow and the nurse on with the babies. Not a very good sign.
The doctor said that one of our babies had just experienced an intraventricular hemmorhage and pulmonary hemmorhage simultaneously. Hearing this was terrifying. The doctor advised us he had actually been at his bedside when the baby started to take a turn for the worse. The baby's appearance had quickly become very ashen (grey) and he appeared to become rigid. That's the way he described it. He didn't go into detail as to whether or not he had physically done something to try to help the baby through it, but realistically I'm not sure that anything can be done in such a situation, except to hope the baby pulls out of it.
As we were only two days into our long stay at the hospital, we were still taking the trip back home nightly, so we felt terrible knowing we were not there when one of our babies was going through one of the biggest challenges of his life at only 2 days old.
I think the shock of being told the details kept me and my husband calm. I rationally asked questions. Why does something like this happen? What does an ultrasound or xray show now? What's the prognosis?
We talked for probably a good forty-five minutes in the private room, just to the side of our twins' bedsides. The social worker took notes. The nurse ensured we understood the doctor's medical lingo and broke things down in layman's terms as needed. The doctor drew diagrams of the brain and the spinal column. He drew a normal brain and the ventricles and an example of how our son's was appearing. His was pretty much filled with blood from the hemmorhage. Now we had to wait and see if the body could naturally clear the ventricle. If the blood could not clear, surgery may be required. A VP (Veintriculoperitoneal) Shunt may need to be inserted by a surgical process.
I remember during this time, the sound of the monitor bell alarms going off was extremely distressing to me in my mind. I didn't want to be sitting in this closed off box of a room. I wanted to be at my twins' bedside and see how the one baby was looking. By this point he was less than the 2 lbs 4 oz he was when he was born. A tiny little skinny thing, with nothing but potential.
Right from the day we arrived in the NICU we had asked the doctor not to scare us with all the maybes, what ifs and possibilities of anything long term for our premature boys. Given this new chain of events, I really wasn't interested in knowing what the future may hold in connection with this new condition we were dealing with. I wanted to deal with the here and now and not the various possible outcomes. We repeated over and over again during our stay, "One day at a time," "One step at a time," "One step forward, two steps back." The third one is really depressing to think about, but various versions of that were said very, very often.
The next three months would be a rollercoaster ride of fear, tears, pride, smiles and at last, relief. Our little man had 2 surgeries before he was 2 months old...before he was even due. He was a fighter and continued to surprise everyone with his ability to recover.
Initially he had a ventricular reservoir inserted into his right front ventricle, which acted as a small place to hold excess cerebral spinal fluid (CSF) and help (a bit) to alleviate some of the intracranial pressure. The fact that the ventricle was blocked was causing the CSF to back up in the brain, causing head swelling. He somewhat resembled The Great Gazoo (you know, from the Flinstones?) His head circumference was enlarged because of the swelling and although it looked terrible, he seemed to be comfortable usually.
The intention of the reservoir was to help extract excess fluid by "tapping" the reservoir every now and then. The hope was that the reservoir would buy time for the body to heal itself. Every time the baby's head/reservoir was tapped, it ran the risk of exposing him to infection. Eventually it got to the point that doing reservoir punctures and lumbar punctures to extract fluid were not productive enough to make doctor's feel a VP Shunt was not needed. So just before his actual due date he had his second surgery and a VP Shunt was inserted.
After surgery he was awake as they wheeled him out in his tiny little plastic transport box on a stretcher. The doctors had said not to expect him to be awake for potentially several hours after the surgery, but there he was looking up at us as they wheeled him out. There was a huge sense of relief.
Unfortunately, about 3 days after his surgery he was so tired out from his surgery and having been put back on full feeds pretty much immediately after surgery (the same day.) It seems we pooped him out and he couldn't handle full feeds and all the energy he needed to keep them up. He was nursing with me and not on a bottle. Eventually, we had to take a nurse's recommendation and get him onto bottle feeds to help him pace himself and possibly be more comfortable at feeding times. He had begun to cough, choke, sputter and forget to breathe when he was nursing and/or bottling. It was so frustrating to have a baby who was nursing 100%, amazingly well the day before surgery, only to have a baby who now had to re-learn it all.
Eventually it got to be that he was losing weight and having such a hard time taking a bottle that he was burning more calories than taking in. At that point in went the NG (naso-gastric) tube into his nose and down to his tummy. Now he was back on "gavage" feeds, running his milk through a syringe and tube into his stomach every three hours. This was disheartning. Depressing. Frustrating. Yet, he began to gain weight again, so at least it was serving a purpose.
Slowly, but surely over another 3 and a half weeks, we worked at getting him to take a bottle and/or nurse effectively. It was a trying time, but I was confident in my skills as a mother and my son's strength, and knew that with the right amount of patience and the right environment we would be fine.
Wow, this is turning into a very long post. I have so much more to say...so I will have to do another blog very soon.
I will continue my story and discuss the discharge, as well as talk about meeting another individual with hydrocephalus who has beaten many odds...
12 Sept 2011
The Apnea, Bradys and Chaos of a NICU, Preemie & Multiple Mom
Given that kids are back to school now, I thought I'd join the crowds and come up with a "scholastic" sounding blog title this week (it has taken me over a week to actually get this done and posted.) I have been back at my full time work for almost two weeks now, which has also added to my serious delay of posting this.
At this time my kids are not actually school age yet, so that's where the school aspect of this blog pretty much stops! Technically, my 3 babies, husband and I are graduates of 3 NICUs, so let's go with that...based on this maybe we should be candidates for an honourary degree somewhere??
The following are the ABCs of life as a mom with premature children, NICU life and twins/3 boys.
Here it goes...
A is for Apnea (of prematurity.) Apnea is when a baby (or person) experiences a pause in breathing that lasts 15-20 seconds, is associated with a baby turning blue/purple or pale and/or is associated with a slowing of the heart rate (called a bradychardia.) Apnea is common in premature infants, as they have not yet developed fully mature lungs, making it more difficult to carry out the process of regular breathing. It can be caused by infection, brain injury, PDA (see below,) low blood sugar, high or low body temperature or insufficient intake of oxygen. Alarms will sound when a baby's oxygen levels dip below their desired settings.
B is for Bilirubin. "What is it? Bilirubin is the byproduct of the body’s recycling of red blood cells. As the excess red blood in the infant’s circulation begin to breakdown in the first few days after birth, they release what is called bilirubin, which causes the yellowish coloring of the skin and eyes. Bilirubin is normally processed by the liver and excreted in the stool. Bilirubin levels in premature infants are often higher because preemies cannot breakdown their red blood cells as fast as a term baby and they’re immature livers cannot excrete the bilirubin as quickly as full term infants can. This becomes a problem because high levels of bilirubin become toxic to the baby’s nervous system. A premature baby’s nervous system is more vulnerable to the toxic effects of bilirubin so it is important that these levels are closely monitored, especially in the first days of life."
From http://www.peekabooicu.net/2011/02/neonatal-jaundice/. "Is Your Fellow Yellow?"
This website is a great resource for family or friends of a NICU baby.
Our 3 preemie boys all bear the small scars of numerous bilirubin heel pricks, which were done to extract blood to assess their Bilirubin levels many times.
C is for CHAOS! Not a day goes by where the house is not a mess, baby bottles are stacking up in the sink or any clean surface waiting to be washed. We are running from appointment to appointment, running... running...running!
D is for DISCHARGE. This refers to the doctor's order to finally send your baby home. One of the most memorable moments of the NICU life. The best moment for sure!
E is for Ears. Getting babies' ears and hearing assessed several times in the first year of life for a very low birth weight child is the norm...or should be. If you haven't had your baby's hearing tested a minimum of two times in the first year (first one while in the NICU) you should ask your pediatrician or doctor following after care to refer you to an audiologist. During the first year of a premature or low birth weight child's life is when hearing impairments may crop up. Best to be safe and check things out.
If your child gets a "refer" following their in NICU hearing test, don't fret. A "refer" is a nice way to say "fail." LOL. Although your child's hearing may be perfectly fine, for some reason the contraption used in the NICU didn't get a very good reading. The reason may be as simple, as the tools weren't used properly (nurses are human too)...maybe something as simple as not being placed in the ear canal properly. One of our children got a "pass," the other a "refer."
F is for Fatigue. I have done the mommy of one premature child experience. I have done the mommy of one 2-year-old + two premature children experience. I jumped from one boy to three boys in less than 2 years. I recall my first maternity leave as a time when I was pretty well-rested, I napped when baby #1 napped in the day, slept in the night when he slept. Our lives were altered, yes, but absolutely nothing like they were altered when baby # 2 and # 3 arrived all together. Fatigue, exhaustion, mentally, physically and emotionally drained are all terms that come to mind. Thankfully our first son is a sound sleeper, who sleeps through the entire night. The twins were the usual kind of babies once home from the NICU. They wanted to eat based on the hospital routine of every three hours. They were conditioned practically from day one to be fed this way. It is alright for a while...but when I was nursing both babies, it was me who had to get up in the night every 3 hours. I would wait until 1:00 AM to go to bed sometimes. Since the babies would have their "last" meal at 9:00 PM, before most people go to bed, I was not ready to be in bed at this time, so I would stay awake until their 12:00 AM feeding time. They'd be done by about 12:30 and I would hit the sack...only to wake up again by about 2:50 to go in get each baby out of bed for 3:00, one after the other, nurse them as quietly and quickly as possible and go back to bed by about 3:45. Of course not every feeding time went off easily or quickly, so sometimes I wasn't getting back to bed even by 4:00...to get up again at 6:00. Most of the time I was so physically exhausted that as soon as my head hit the pillow, I'd be sound asleep. I was probably half sleepwalking to begin with on many nights, to and from the babies' room. These days, now that we are done with nursing and they are eating solids and having maybe 4 or 5 bottles a day, we are all pretty well-rested. Thankfully, I have 3 sound sleeping little boys.
G is for Gavage feeding. A gavage feeding is the practice of feeding a baby by pouring formula or breastmilk into a syringe, which is attached to either a NG (Naso-Gastric) Tube, which goes through the nose to the stomach or an OG (Oro-Gastric) Tube, which goes through the mouth to the stomach. Gavage feeds are often done when a baby is not yet strong enough to nurse or take a bottle. Sometimes it is used to help supplement feeds. They are often used in the early days when a mother is not able to be at bedside around the clock, especially in the late night/early morning hours.
H is for Hemmorhage...intraventricular (brain)...pulmonary (lungs)...It is not exactly known why preemies tend to suffer brain or pulmonary hemmorhages. It is thought that if the child had a traumatic delivery, this could play a role. If the baby was born in a hurry, such as my 3, then they may have had a bit of bumping around or pressure do to their quick exit. It is hard for doctors to be 100% certain. My Baby B was turned by the doctor, using an external method with his hands on my stomach. Perhaps this is why he had his intraventricular hemmorhage. We will never know. An IVH can lead to Hydrocephalus (another H,) which simply put, is the build of up Cerebral Spinal Fluid (CSF) in the brain, which is unable to naturally flow up and down the spinal column. Blood remnants following an IVH, can "clog" the process, causing brain swelling and most likely surgery.
I is for Indomethacin vs. Ibuprofen. Two drugs used to attempt to close a Patent Ductus Arteriosus. The PDA is a heart defect that is identified when the Ductus Arteriosus does not shut within a few days after birth. It is more common for premature infants to have a problem with this duct shutting and it is often medicated to try to assist in its closure with either Indomethicin or Ibuprofen (not the kind in your cupboards!) It depends on the hospital's opinion or protocol as to which medication type they will use. A more detailed description of the PDA and why this is a problem can be found here http://www.nhlbi.nih.gov/health/health-topics/topics/pda/.
J is for Jack of All Trades. As a preemie/NICU mom you will become your child's (childrens') advocate. You will begin to develop a wealth of knowledge in all areas...areas which you never even knew existed before arriving in your current situation. I, myself, have become familiar with NICU medical jargon, health conditions, developmental stages, social services available, assisted services available and all kinds of medical professions. This is why you will become a Jack of All Trades (Master of A LOT!)
K is for Kilogram. This is a measurement of weight we refer to in Canada...The metric system. Although the majority of the world uses the metric system, you will still find many of us Canadians talking pounds and ounces and looking very perplexed when someone throws out a weight in kilograms.
L is for Lumbar puncture. A lumbar puncture is a process of withdrawing cerebral spinal fluid from the spinal column. The puncture is done with a needle being inserted into the lower area of the spinal column. The fluid is extracted for the purpose of checking for infection or to alleviate excess CSF buildup in the spinal column/brain, which will cause hydrocephalus (fluid buildup in the brain's ventricles.)
M is for Monitor. If you have never been in a NICU, it would be hard to understand how to this day a parent that has been in a NICU can recall the exact sound of alarming monitors. From the slow dings to the repetitive, very fast pace dings, the sound can make the hair on the back of your neck stand up. A parent that is new to the NICU will feel like they are on pins and needles when alarms are sounding. Soon a parent will become accustomed to what the slow dings mean to the fast paced "get over here now" alarms mean. It doesn't mean you are ever really 100% comfortable with the sounds constantly going on around you.
N is for Nurse, of course. The nursing staff in tertiary NICUs are the best of the best. They have excellent educational backgrounds and extensive hands on training and knowledge prior to moving into a NICU.
O is for Occupational Therapy. The OT is a person that assesses a baby's neurologic development (brain) and helps implement plans to assist a baby's overall development, improve a baby's muscle control and address possible feeding problems. All three of our boys had an OT while in the NICU. Baby #3 had the most attention from an OT. Following his second surgery for hydrocephalus, he forgot how to eat! He needed help with positioning his head on a butterfly pillow. He needed help with learning how to "suck, swallow, breathe" again while nursing or bottling. He had to learn to hold his head with a shunt. It was very difficult to watch and go through with our little guy. The OT made it easier with many comments, suggestions and a listening ear. It was like we were a team, trying to think up the best ways to get this little boy to develop well and get the heck out of that hospital as soon as possible. The final thing holding us back from going home was to get him to remember how to "suck, swallow and breathe."
P is for Physiotherapy. This is a specialist that pays attention to a baby's coordination and large motor skills development. Thankfully, we were referred to physiotherapy and occupational therapy even before discharge. Due to our twins very premature arrival, it was expected that the babies would most likely need some assistance with their development over the first few years.
Q is for Questions. You will have lots of them when staying in a NICU...so ask them!
R is for Respiratory Therapist. Most premature infants will have some form of respiratory distress. My babies did very shortly after birth and were required to be "bagged" and then intubated. Bagged is a layman's term to describe a means to slowly, rhytmically provide oxygen into the baby's lungs using what looks like a small balloon, manually squeezing air into the airway. Intubation is usually the last approach to assist the baby with breathing. A tube is inserted through the nose or mouth and down the back of the throat into the airway. The tube will most likely be there for a little while, until the baby proves he or she can breathe on his/her own or until another method can be tried, such as CPAP. The Respiratory Therapist (RT) will monitor the babies breathing, their patterns, monitor settings and adjust for the baby's needs. Many premature babies will suffer from some level of Respiratory Distress Syndrome. The ultimate goal is to gradually get the baby ready to breathe "room air," which means to be off any sort of "respiratory support," and breathe all on their own.
S is for Sepsis Neonatorum, which is an infection of the newborn "that spreads throughout the baby’s body. Sepsis occurs in less than 1 percent of newborns (1 out of every 100), but accounts for up to 30 percent of deaths in the first few weeks of life. Infection is 5-10 times more common in premature newborns and in babies weighing less than 5½ pounds than in normal-weight, full-term newborns. Complications experienced during birth, such as premature or prolonged rupture of the membranes or infection in the mother, put the newborn at increased risk of infection...The onset of what is called early-onset neonatal sepsis is within six hours of birth in over half the cases and within 72 hours in the great majority of cases. Sepsis that begins four or more days after birth is called late-onest sepsis, and is probably an infection acquired in the hospital nursery (a nosocomial infection). In both types of neonatal sepsis, the infection may be only in the bloodstream, or may spread to the lungs (pneumonia), brain (meningitis), bone (osteomyelitis), joints, or other organs in the body." Children's Specialists of San Diego.
Antibiotics are often started even before a formal lab report is returned, because sometimes there is no choice or it is not wise to wait. Should the child be shown to be clear of sepsis, then the antibiotics regimine would be stopped, with no harm done.
T is for Transfusion. A premature infant is very susceptible to developing low hemoglobin counts, which can lead to the need for blood transfusions. Sometimes many. Red blood cells carry hemoglobin, which contains iron and carries oxygen, and if their counts are too low babies will become anemic. The doctors and staff will monitor a baby's levels. Sometimes it will seem as though it has taken only a few hours for your child's appearance to degrade severely. A baby may appear ashen or extremely pale in colour. It can be a scary thing to see. This happened to us on several occasions with both of the twins. It got to the point sometimes that we would start telling the nurses, "it looks like his hemoglobin has dropped again." Sometimes it was so apparent, but we were told that sometimes the body corrects this problem on its own. The doctors didn't immediately order blood transfusions at first glance. They usually gave the body time to sort itself out.
U is for Ultrasound. As we all know a pregnancy means you will most likely have at least one ultrasound before the arrival of your baby. If you're carrying multiples you will have a minimum of one ultrasound, but most likely, you'll have several. Since I was already high risk for having a second premature baby, I had my first ultrasound at 12 weeks for screening and to assess the exact number of weeks of gestation. Once we found out I was having twins at that ultrasound appointment, I was scheduled for one ultrasound every month until the babies were born. All three babies had many ultrasounds while in hospital. Of the brain, of the heart, of the kidneys...whatever they wanted to make sure was doing okay, they did an ultrasound on it.
V is for VICTORY. I can't imagine feeling more victorious, than when a parent/family walks out of a NICU after a long stay. Our babies may have some battle wounds, but they made it. They are strong and they are fighters.
W is for WBC (White Blood Cells). White blood cells help the body fight against infection. Often premature infants WBC count can become dangerously low, leaving the body unable to fight effectively against potential infection.
X is for XRAY. A premature baby will most likely have many XRAYS during their NICU stay.
Y is for Yup, I'm running out of words to work with here...
Z is for Zzzzzzz...
At this time my kids are not actually school age yet, so that's where the school aspect of this blog pretty much stops! Technically, my 3 babies, husband and I are graduates of 3 NICUs, so let's go with that...based on this maybe we should be candidates for an honourary degree somewhere??
The following are the ABCs of life as a mom with premature children, NICU life and twins/3 boys.
Here it goes...
A is for Apnea (of prematurity.) Apnea is when a baby (or person) experiences a pause in breathing that lasts 15-20 seconds, is associated with a baby turning blue/purple or pale and/or is associated with a slowing of the heart rate (called a bradychardia.) Apnea is common in premature infants, as they have not yet developed fully mature lungs, making it more difficult to carry out the process of regular breathing. It can be caused by infection, brain injury, PDA (see below,) low blood sugar, high or low body temperature or insufficient intake of oxygen. Alarms will sound when a baby's oxygen levels dip below their desired settings.
B is for Bilirubin. "What is it? Bilirubin is the byproduct of the body’s recycling of red blood cells. As the excess red blood in the infant’s circulation begin to breakdown in the first few days after birth, they release what is called bilirubin, which causes the yellowish coloring of the skin and eyes. Bilirubin is normally processed by the liver and excreted in the stool. Bilirubin levels in premature infants are often higher because preemies cannot breakdown their red blood cells as fast as a term baby and they’re immature livers cannot excrete the bilirubin as quickly as full term infants can. This becomes a problem because high levels of bilirubin become toxic to the baby’s nervous system. A premature baby’s nervous system is more vulnerable to the toxic effects of bilirubin so it is important that these levels are closely monitored, especially in the first days of life."
From http://www.peekabooicu.net/2011/02/neonatal-jaundice/. "Is Your Fellow Yellow?"
This website is a great resource for family or friends of a NICU baby.
Our 3 preemie boys all bear the small scars of numerous bilirubin heel pricks, which were done to extract blood to assess their Bilirubin levels many times.
C is for CHAOS! Not a day goes by where the house is not a mess, baby bottles are stacking up in the sink or any clean surface waiting to be washed. We are running from appointment to appointment, running... running...running!
D is for DISCHARGE. This refers to the doctor's order to finally send your baby home. One of the most memorable moments of the NICU life. The best moment for sure!
E is for Ears. Getting babies' ears and hearing assessed several times in the first year of life for a very low birth weight child is the norm...or should be. If you haven't had your baby's hearing tested a minimum of two times in the first year (first one while in the NICU) you should ask your pediatrician or doctor following after care to refer you to an audiologist. During the first year of a premature or low birth weight child's life is when hearing impairments may crop up. Best to be safe and check things out.
If your child gets a "refer" following their in NICU hearing test, don't fret. A "refer" is a nice way to say "fail." LOL. Although your child's hearing may be perfectly fine, for some reason the contraption used in the NICU didn't get a very good reading. The reason may be as simple, as the tools weren't used properly (nurses are human too)...maybe something as simple as not being placed in the ear canal properly. One of our children got a "pass," the other a "refer."
F is for Fatigue. I have done the mommy of one premature child experience. I have done the mommy of one 2-year-old + two premature children experience. I jumped from one boy to three boys in less than 2 years. I recall my first maternity leave as a time when I was pretty well-rested, I napped when baby #1 napped in the day, slept in the night when he slept. Our lives were altered, yes, but absolutely nothing like they were altered when baby # 2 and # 3 arrived all together. Fatigue, exhaustion, mentally, physically and emotionally drained are all terms that come to mind. Thankfully our first son is a sound sleeper, who sleeps through the entire night. The twins were the usual kind of babies once home from the NICU. They wanted to eat based on the hospital routine of every three hours. They were conditioned practically from day one to be fed this way. It is alright for a while...but when I was nursing both babies, it was me who had to get up in the night every 3 hours. I would wait until 1:00 AM to go to bed sometimes. Since the babies would have their "last" meal at 9:00 PM, before most people go to bed, I was not ready to be in bed at this time, so I would stay awake until their 12:00 AM feeding time. They'd be done by about 12:30 and I would hit the sack...only to wake up again by about 2:50 to go in get each baby out of bed for 3:00, one after the other, nurse them as quietly and quickly as possible and go back to bed by about 3:45. Of course not every feeding time went off easily or quickly, so sometimes I wasn't getting back to bed even by 4:00...to get up again at 6:00. Most of the time I was so physically exhausted that as soon as my head hit the pillow, I'd be sound asleep. I was probably half sleepwalking to begin with on many nights, to and from the babies' room. These days, now that we are done with nursing and they are eating solids and having maybe 4 or 5 bottles a day, we are all pretty well-rested. Thankfully, I have 3 sound sleeping little boys.
G is for Gavage feeding. A gavage feeding is the practice of feeding a baby by pouring formula or breastmilk into a syringe, which is attached to either a NG (Naso-Gastric) Tube, which goes through the nose to the stomach or an OG (Oro-Gastric) Tube, which goes through the mouth to the stomach. Gavage feeds are often done when a baby is not yet strong enough to nurse or take a bottle. Sometimes it is used to help supplement feeds. They are often used in the early days when a mother is not able to be at bedside around the clock, especially in the late night/early morning hours.
H is for Hemmorhage...intraventricular (brain)...pulmonary (lungs)...It is not exactly known why preemies tend to suffer brain or pulmonary hemmorhages. It is thought that if the child had a traumatic delivery, this could play a role. If the baby was born in a hurry, such as my 3, then they may have had a bit of bumping around or pressure do to their quick exit. It is hard for doctors to be 100% certain. My Baby B was turned by the doctor, using an external method with his hands on my stomach. Perhaps this is why he had his intraventricular hemmorhage. We will never know. An IVH can lead to Hydrocephalus (another H,) which simply put, is the build of up Cerebral Spinal Fluid (CSF) in the brain, which is unable to naturally flow up and down the spinal column. Blood remnants following an IVH, can "clog" the process, causing brain swelling and most likely surgery.
I is for Indomethacin vs. Ibuprofen. Two drugs used to attempt to close a Patent Ductus Arteriosus. The PDA is a heart defect that is identified when the Ductus Arteriosus does not shut within a few days after birth. It is more common for premature infants to have a problem with this duct shutting and it is often medicated to try to assist in its closure with either Indomethicin or Ibuprofen (not the kind in your cupboards!) It depends on the hospital's opinion or protocol as to which medication type they will use. A more detailed description of the PDA and why this is a problem can be found here http://www.nhlbi.nih.gov/health/health-topics/topics/pda/.
J is for Jack of All Trades. As a preemie/NICU mom you will become your child's (childrens') advocate. You will begin to develop a wealth of knowledge in all areas...areas which you never even knew existed before arriving in your current situation. I, myself, have become familiar with NICU medical jargon, health conditions, developmental stages, social services available, assisted services available and all kinds of medical professions. This is why you will become a Jack of All Trades (Master of A LOT!)
K is for Kilogram. This is a measurement of weight we refer to in Canada...The metric system. Although the majority of the world uses the metric system, you will still find many of us Canadians talking pounds and ounces and looking very perplexed when someone throws out a weight in kilograms.
L is for Lumbar puncture. A lumbar puncture is a process of withdrawing cerebral spinal fluid from the spinal column. The puncture is done with a needle being inserted into the lower area of the spinal column. The fluid is extracted for the purpose of checking for infection or to alleviate excess CSF buildup in the spinal column/brain, which will cause hydrocephalus (fluid buildup in the brain's ventricles.)
M is for Monitor. If you have never been in a NICU, it would be hard to understand how to this day a parent that has been in a NICU can recall the exact sound of alarming monitors. From the slow dings to the repetitive, very fast pace dings, the sound can make the hair on the back of your neck stand up. A parent that is new to the NICU will feel like they are on pins and needles when alarms are sounding. Soon a parent will become accustomed to what the slow dings mean to the fast paced "get over here now" alarms mean. It doesn't mean you are ever really 100% comfortable with the sounds constantly going on around you.
N is for Nurse, of course. The nursing staff in tertiary NICUs are the best of the best. They have excellent educational backgrounds and extensive hands on training and knowledge prior to moving into a NICU.
O is for Occupational Therapy. The OT is a person that assesses a baby's neurologic development (brain) and helps implement plans to assist a baby's overall development, improve a baby's muscle control and address possible feeding problems. All three of our boys had an OT while in the NICU. Baby #3 had the most attention from an OT. Following his second surgery for hydrocephalus, he forgot how to eat! He needed help with positioning his head on a butterfly pillow. He needed help with learning how to "suck, swallow, breathe" again while nursing or bottling. He had to learn to hold his head with a shunt. It was very difficult to watch and go through with our little guy. The OT made it easier with many comments, suggestions and a listening ear. It was like we were a team, trying to think up the best ways to get this little boy to develop well and get the heck out of that hospital as soon as possible. The final thing holding us back from going home was to get him to remember how to "suck, swallow and breathe."
P is for Physiotherapy. This is a specialist that pays attention to a baby's coordination and large motor skills development. Thankfully, we were referred to physiotherapy and occupational therapy even before discharge. Due to our twins very premature arrival, it was expected that the babies would most likely need some assistance with their development over the first few years.
Q is for Questions. You will have lots of them when staying in a NICU...so ask them!
R is for Respiratory Therapist. Most premature infants will have some form of respiratory distress. My babies did very shortly after birth and were required to be "bagged" and then intubated. Bagged is a layman's term to describe a means to slowly, rhytmically provide oxygen into the baby's lungs using what looks like a small balloon, manually squeezing air into the airway. Intubation is usually the last approach to assist the baby with breathing. A tube is inserted through the nose or mouth and down the back of the throat into the airway. The tube will most likely be there for a little while, until the baby proves he or she can breathe on his/her own or until another method can be tried, such as CPAP. The Respiratory Therapist (RT) will monitor the babies breathing, their patterns, monitor settings and adjust for the baby's needs. Many premature babies will suffer from some level of Respiratory Distress Syndrome. The ultimate goal is to gradually get the baby ready to breathe "room air," which means to be off any sort of "respiratory support," and breathe all on their own.
S is for Sepsis Neonatorum, which is an infection of the newborn "that spreads throughout the baby’s body. Sepsis occurs in less than 1 percent of newborns (1 out of every 100), but accounts for up to 30 percent of deaths in the first few weeks of life. Infection is 5-10 times more common in premature newborns and in babies weighing less than 5½ pounds than in normal-weight, full-term newborns. Complications experienced during birth, such as premature or prolonged rupture of the membranes or infection in the mother, put the newborn at increased risk of infection...The onset of what is called early-onset neonatal sepsis is within six hours of birth in over half the cases and within 72 hours in the great majority of cases. Sepsis that begins four or more days after birth is called late-onest sepsis, and is probably an infection acquired in the hospital nursery (a nosocomial infection). In both types of neonatal sepsis, the infection may be only in the bloodstream, or may spread to the lungs (pneumonia), brain (meningitis), bone (osteomyelitis), joints, or other organs in the body." Children's Specialists of San Diego.
Antibiotics are often started even before a formal lab report is returned, because sometimes there is no choice or it is not wise to wait. Should the child be shown to be clear of sepsis, then the antibiotics regimine would be stopped, with no harm done.
T is for Transfusion. A premature infant is very susceptible to developing low hemoglobin counts, which can lead to the need for blood transfusions. Sometimes many. Red blood cells carry hemoglobin, which contains iron and carries oxygen, and if their counts are too low babies will become anemic. The doctors and staff will monitor a baby's levels. Sometimes it will seem as though it has taken only a few hours for your child's appearance to degrade severely. A baby may appear ashen or extremely pale in colour. It can be a scary thing to see. This happened to us on several occasions with both of the twins. It got to the point sometimes that we would start telling the nurses, "it looks like his hemoglobin has dropped again." Sometimes it was so apparent, but we were told that sometimes the body corrects this problem on its own. The doctors didn't immediately order blood transfusions at first glance. They usually gave the body time to sort itself out.
U is for Ultrasound. As we all know a pregnancy means you will most likely have at least one ultrasound before the arrival of your baby. If you're carrying multiples you will have a minimum of one ultrasound, but most likely, you'll have several. Since I was already high risk for having a second premature baby, I had my first ultrasound at 12 weeks for screening and to assess the exact number of weeks of gestation. Once we found out I was having twins at that ultrasound appointment, I was scheduled for one ultrasound every month until the babies were born. All three babies had many ultrasounds while in hospital. Of the brain, of the heart, of the kidneys...whatever they wanted to make sure was doing okay, they did an ultrasound on it.
V is for VICTORY. I can't imagine feeling more victorious, than when a parent/family walks out of a NICU after a long stay. Our babies may have some battle wounds, but they made it. They are strong and they are fighters.
W is for WBC (White Blood Cells). White blood cells help the body fight against infection. Often premature infants WBC count can become dangerously low, leaving the body unable to fight effectively against potential infection.
X is for XRAY. A premature baby will most likely have many XRAYS during their NICU stay.
Y is for Yup, I'm running out of words to work with here...
Z is for Zzzzzzz...
Labels:
Apnea,
gavage,
hydrocephalus,
ibuprofen,
indomethacin,
Jack of All Trades,
kilogram,
Lumbar puncture,
monitor,
OT,
PT,
Respiratory Distress Syndrome,
Sepsis,
transfusion,
ultrasound,
VICTORY
31 Aug 2011
Hi-ho! Hi-ho! It's Off to Work I Go!
Today, after 16 months, I re-joined the morning rush hour to head into work.
I had planned and re-planned my first day back to work in my head and how I would strategically pull off having a shower, drying my hair, and straigthtening my hair all before the twins woke up. (Big brother was at his grandmother's house for the night to help us out a bit.) In my mind I would get these three tasks done and then get the babies up, put them in their high chairs with their morning bottle, get their daytime bottles mixed up for the babysitter, feed the babies, then get dressed afterward to ensure I didn't get any baby splatter on my good work clothes.
Last night I triple-checked that my TV alarm would click on at the right time. Checked that the time on the TV was actually set for AM and not PM and so on. I didn't want to screw up my first morning back to work!
My sleep was restless and even though I didn't feel stressed out or worried about my first day back, I think just the idea of sleeping in and ruining "The Plan," was keeping me from sleeping well. When I say, "sleeping in," all I really mean is sleeping to our usual 7:15 or 7:30, which would have had me at least 45 minutes behind schedule. Not good!
Twin A had other ideas anyway and he let it be known at 5:55 AM that he was ready to get up. This was so unusual for him to do and I really do think that he could tell something was up. These babies usually sleep at least 11 hours! There he was in bed, jibber jabbering away, waiting for someone to come get him.
"The Plan" was already destroyed! I hadn't even gotten out of bed yet! :) Instead, both babies had their bottles in bed, which their Daddy made, while I had a shower. Amazingly, we were able to pull off the rest of "The Plan," getting them fed in their high chairs and getting dressed and out the door at 7:43...2 minutes ahead of schedule. *Big Smiles*
We got the babies over to their babysitter's house at 8:00 on the dot. My hubby joined me to officially meet the babysitter and know where to go in the event of a "please come pick up your kid" request, if I couldn't deal with a potential problem with one of the kids!
Off my husband and I went in different directions after dropping off the twins and I made it to my office with ten minutes to spare before the official start of my day.
My first day back went very well. I felt right at home again, as though I hadn't actually been gone all this time. Since the twins arrived so early, 16 months ago, I really hadn't had the opportunity to do the usual slow wind down and wrap up of my job all those months ago. One day I was there, the next I wasn't. I think this is why I felt like I hadn't actually been gone that long. My memories of the final few days at work before my sudden departure were very fresh in my mind. I can remember several of the clients I was working with, conversations I had been having with them and so on. It's kind of like my work-life was at a stand-still in my mind...but in reality, my how things have changed!
I have a lot of new things to learn and I will definitely be kept on my toes over the next few weeks, learning the many changes that have occurred over the last year and a bit. I think I will be hitting the sack as soon as I can when I come home in the evenings because all this new information is going to be draining. I am, however, looking forward to taking on this renewed challenge! Today sped by very quickly, which I was amazed by. I was reading, refreshing my memory, and learning new things so quickly, so I didn't have time to stop and look at the clock all that much.
I did pull a few serious mommy-brained moves today and one for sure left at least one co-worker scratching her head. Hehehe. First off, I forgot my wallet and had no lunch prepared and no lunch money, so I had to drive back home to get my wallet. Once home I ate leftovers from the fridge, so that worked out okay. I drove back to work and parked in a temporary parking spot, so I could carry in one of my work boxes I had brought home during my mat leave. I left my driver's side door open, while I went to the back and got my box out of the trunk. I then set the box down on the curb next to me and opened the front passenger door, grabbed my nice steamy Tim Hortons coffee, shut the door, armed the car with my remote key and walked away.
About 20 minutes later I received my first phone call on my office extension and it was my co-worker friend, asking if everything was alright. Of course it is, I said...why?? She tells me she was worried about me because she just passed my car and saw the driver's door wide open, but I wasn't anywhere to be seen!! What??!! Did you shut it, I asked? No! What?!?! OH MY GOD!! I had to run for it as fast as possible, which is next to impossible in the style of thong sandal shoes I was wearing! How ridiculous! Why would my van remote lock thingy "honk" when I thought I was locking up all the doors, while one door hung wide open? That makes no sense to me. Like I said before, I am not really a fan of my van...so this just adds to my lists of why not to like this van! Yes, it was really dumb of me to leave the door wide open, but why did the locks engage and the van "honk" if it wasn't really secured? No sense...
The van was fine, my change still remained in the change slots, my parking pass was not stolen, and most importantly, my 3 kids' carseats were still in there, nice and secure. All I could envision as I ran to my van was having to replace $700+ in carseats!
I do have to wonder why the person who parked next to my van didn't bother to shut it. I also wonder if they reported to anyone at City Hall, where I was parked, that their was a suspicious van in the parking lot. I wonder. I imagine that everyone minded their own business and went about life like nothing was out of the ordinary. I think that's pretty sad.
My co-worker said she didn't shut the door because she didn't want to put fingerprints on the door, in case there really was something wrong! I hear that. I get that. She did call me and found I was okay. That's cool.
Anyway, those were my two mommy-brain episodes today on my first day back to work. The bottom line is I did make it to work on time, my twin babies were content at their babysitter's, eldest son had an awesome time at a pool with his grandmother and my hubby and I were able to work so well together this morning and this evening to make our new reality work! I also got a parting gift this evening from the babysitter, which was fresh mini meringues with custard and fruit on top. I think I should move into this woman's house...I'd eat really well!
I had planned and re-planned my first day back to work in my head and how I would strategically pull off having a shower, drying my hair, and straigthtening my hair all before the twins woke up. (Big brother was at his grandmother's house for the night to help us out a bit.) In my mind I would get these three tasks done and then get the babies up, put them in their high chairs with their morning bottle, get their daytime bottles mixed up for the babysitter, feed the babies, then get dressed afterward to ensure I didn't get any baby splatter on my good work clothes.
Last night I triple-checked that my TV alarm would click on at the right time. Checked that the time on the TV was actually set for AM and not PM and so on. I didn't want to screw up my first morning back to work!
My sleep was restless and even though I didn't feel stressed out or worried about my first day back, I think just the idea of sleeping in and ruining "The Plan," was keeping me from sleeping well. When I say, "sleeping in," all I really mean is sleeping to our usual 7:15 or 7:30, which would have had me at least 45 minutes behind schedule. Not good!
Twin A had other ideas anyway and he let it be known at 5:55 AM that he was ready to get up. This was so unusual for him to do and I really do think that he could tell something was up. These babies usually sleep at least 11 hours! There he was in bed, jibber jabbering away, waiting for someone to come get him.
"The Plan" was already destroyed! I hadn't even gotten out of bed yet! :) Instead, both babies had their bottles in bed, which their Daddy made, while I had a shower. Amazingly, we were able to pull off the rest of "The Plan," getting them fed in their high chairs and getting dressed and out the door at 7:43...2 minutes ahead of schedule. *Big Smiles*
We got the babies over to their babysitter's house at 8:00 on the dot. My hubby joined me to officially meet the babysitter and know where to go in the event of a "please come pick up your kid" request, if I couldn't deal with a potential problem with one of the kids!
Off my husband and I went in different directions after dropping off the twins and I made it to my office with ten minutes to spare before the official start of my day.
My first day back went very well. I felt right at home again, as though I hadn't actually been gone all this time. Since the twins arrived so early, 16 months ago, I really hadn't had the opportunity to do the usual slow wind down and wrap up of my job all those months ago. One day I was there, the next I wasn't. I think this is why I felt like I hadn't actually been gone that long. My memories of the final few days at work before my sudden departure were very fresh in my mind. I can remember several of the clients I was working with, conversations I had been having with them and so on. It's kind of like my work-life was at a stand-still in my mind...but in reality, my how things have changed!
I have a lot of new things to learn and I will definitely be kept on my toes over the next few weeks, learning the many changes that have occurred over the last year and a bit. I think I will be hitting the sack as soon as I can when I come home in the evenings because all this new information is going to be draining. I am, however, looking forward to taking on this renewed challenge! Today sped by very quickly, which I was amazed by. I was reading, refreshing my memory, and learning new things so quickly, so I didn't have time to stop and look at the clock all that much.
I did pull a few serious mommy-brained moves today and one for sure left at least one co-worker scratching her head. Hehehe. First off, I forgot my wallet and had no lunch prepared and no lunch money, so I had to drive back home to get my wallet. Once home I ate leftovers from the fridge, so that worked out okay. I drove back to work and parked in a temporary parking spot, so I could carry in one of my work boxes I had brought home during my mat leave. I left my driver's side door open, while I went to the back and got my box out of the trunk. I then set the box down on the curb next to me and opened the front passenger door, grabbed my nice steamy Tim Hortons coffee, shut the door, armed the car with my remote key and walked away.
About 20 minutes later I received my first phone call on my office extension and it was my co-worker friend, asking if everything was alright. Of course it is, I said...why?? She tells me she was worried about me because she just passed my car and saw the driver's door wide open, but I wasn't anywhere to be seen!! What??!! Did you shut it, I asked? No! What?!?! OH MY GOD!! I had to run for it as fast as possible, which is next to impossible in the style of thong sandal shoes I was wearing! How ridiculous! Why would my van remote lock thingy "honk" when I thought I was locking up all the doors, while one door hung wide open? That makes no sense to me. Like I said before, I am not really a fan of my van...so this just adds to my lists of why not to like this van! Yes, it was really dumb of me to leave the door wide open, but why did the locks engage and the van "honk" if it wasn't really secured? No sense...
The van was fine, my change still remained in the change slots, my parking pass was not stolen, and most importantly, my 3 kids' carseats were still in there, nice and secure. All I could envision as I ran to my van was having to replace $700+ in carseats!
I do have to wonder why the person who parked next to my van didn't bother to shut it. I also wonder if they reported to anyone at City Hall, where I was parked, that their was a suspicious van in the parking lot. I wonder. I imagine that everyone minded their own business and went about life like nothing was out of the ordinary. I think that's pretty sad.
My co-worker said she didn't shut the door because she didn't want to put fingerprints on the door, in case there really was something wrong! I hear that. I get that. She did call me and found I was okay. That's cool.
Anyway, those were my two mommy-brain episodes today on my first day back to work. The bottom line is I did make it to work on time, my twin babies were content at their babysitter's, eldest son had an awesome time at a pool with his grandmother and my hubby and I were able to work so well together this morning and this evening to make our new reality work! I also got a parting gift this evening from the babysitter, which was fresh mini meringues with custard and fruit on top. I think I should move into this woman's house...I'd eat really well!
Subscribe to:
Posts (Atom)






